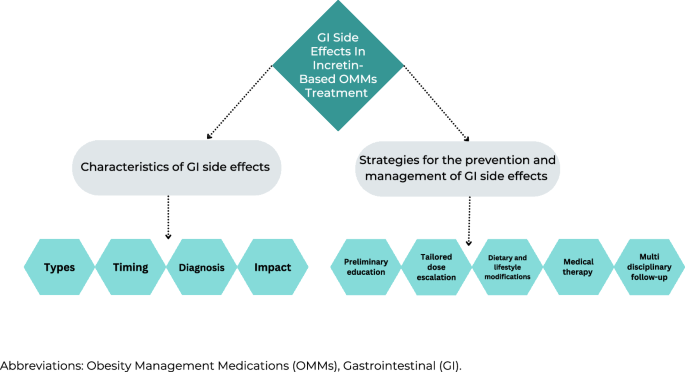
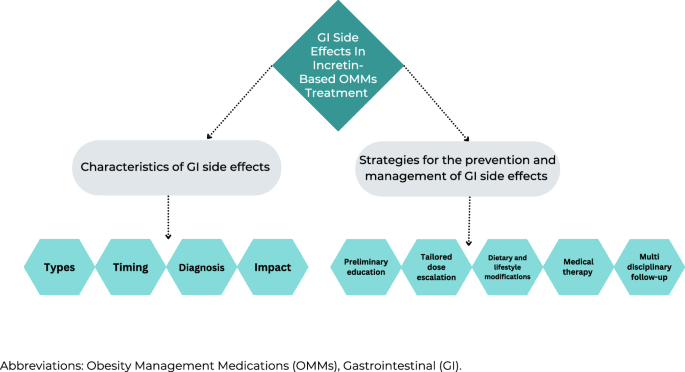
The results yielded two main themes that emerged from the patient’s interviews and HCPs focus groups analysis (Fig. 1). The first theme focuses on the different characteristics of GI side effects from a dual perspective of both HCPs and patients, encompassing four sub-themes: (1) types of common GI side effects, (2) the timing of GI side effect events (3) challenges in diagnosis, and (4) their impact on quality of life and treatment adherence. The second theme focuses on strategies for the prevention and management of GI side effects during incretin-based OMMs treatment encompassing five sub-themes: (1) preliminary education, (2) tailored dose escalation, (3) dietary and lifestyle modifications for the treatment of specific GI symptoms, (4) medical therapy to alleviate symptoms, and (5) the importance of multidisciplinary care follow-up.
Characteristics of GI side effects in incretin-based OMM treatment
This theme primarily focuses on different characteristics of GI side effects from a dual perspective of both HCPs and patients receiving incretin-based OMM therapy.
Types of GI side effects
There is variability in the types and severity of GI side effects associated with incretin-based OMMs as described by both patients and HCPs. Common side effects primarily involved the upper GI system, with nausea being particularly frequent. Another commonly reported side effect, noted by both HCPs and patients, is belching, often described as having a strong odor and occasionally an unpleasant taste. Vomiting is considered an infrequent side effect according to HCPs and may occur in situations of excessively rapid increases in medication dosage or eating large amounts of food unsuitable for delayed gastric emptying. For the lower GI system, diarrhea and constipation were identified by both HCPs and patients as the most common side effects. Generally, diarrhea was described as occurring with relative urgency and intensity but for a limited duration, whereas constipation was described as less intense but more prolonged. Additional common GI side effects reported by both HCPs and patients include heartburn, abdominal pain, flatulence, and bloating.
Timing of GI side effects
Most HCPs and patients indicated that GI side effects occur primarily at the initiation of treatment and/or following dose escalation during the titration phase. Both HCPs and patients also noted a gradual improvement in GI side effects occurrence and severity with continued medication use.
Furthermore, some demonstrated an “element of surprise” regarding the timing of GI side effects. On the one hand, certain GI side effects were reported to occur on a specific period after the injection of the medication, allowing patients to anticipate them and therefore describing them as tolerable (“living with it”). Conversely, certain GI side effects, particularly diarrhea, can arise suddenly and urgently, often without warning, even after several months of medication use. One dietitian shared from her clinical experience:
“The sudden and urgency of bowel movements is something that greatly disturbs patients and represents their primary fear of what will happen after taking the medication.” (Participant# 6, dietitian).
Two patients highlighted the unexpected nature of diarrhea and belching as well:
“ Just when you think it’s over, it hits you out of nowhere – an urgent bathroom need. If you’re not near one, you’d better have spare clothes handy.” (Patient number #8).
“What bothers me are these small belches that can ambush you in the middle of a conversation. It’s embarrassing because it suddenly comes out of nowhere and is completely unexpected.” (Patient number #4).
Diagnosis—between GI side effects and normal medication effects
Interviews with HCPs and patients highlight the challenge of understanding how novel medications affect the body and differentiating normal drug effects from abnormal GI side effects. One contributing factor is the unfamiliar sensations induced by the medication as one dietitian described:
“Some patients report an uncomfortable sensation as if something is stuck. This is an unfamiliar and novel sensation, unlike side effects such as diarrhea or constipation.” (Participant# 6, dietitian).
A patient also shared the same experience:
“I know nausea, and this isn’t it. It’s some constant, undefined discomfort – not fullness, but something that keeps me from eating.” (Patient number #5).
The impact of GI side effects on quality of life and treatment adherence
Most patients characterized GI side effects as unpleasant but manageable, describing their impact on quality of life as moderate and generally tolerable.
Notably, many patients are willing to ‘pay the price’ of GI side effects to lose weight and improve their obesity related medical condition, a perspective often distinct from those with other chronic conditions. One of the physicians shared her impression:
“People with obesity are willing to suffer more than those with diabetes because if they believe you’re giving them something that will help them lose weight, they’ll do a lot for it. They’ll even agree to endure diarrhea.” (Participant# 1, physician).
Another dietitian added:
“Some patients are willing to suffer side effects and continue the treatment because they perceive their obesity, diabetes, or fatty liver is more severe than GI side effects.” (Participant# 6, dietitian).
Similarly, patients emphasized the significance of obesity treatment and expressed their willingness to “make sacrifices” for its success, including tolerating side effects as one patient stated:
“I felt that whatever this medication would throw at me, I could handle it, just as long as I didn’t gain weight. If I need to lose weight or prevent liver problems, that’s my top priority. How comfortable my stomach feels is somewhere five places below that.” (Patient number #8).
According to HCPs, patients with multidisciplinary support, primarily a physician and a dietitian, rarely quit treatment due to GI side effects. One physician provided an example illustrating how the lack of multidisciplinary support contributes to medication discontinuation among patients in community settings:
“Many of my patients come after failing elsewhere with OMMs. They got prescriptions from primary care doctors but were left without proper follow-up. Without professional monitoring, they just suffered and quit. They arrive frustrated from these experiences.” (Participant# 2, physician).
Strategies for prevention and management of GI side effects
This theme explores the lived experiences and shared insights regarding prevention and management strategies of GI side effects, emerging from the dual perspectives of HCPs and patients receiving incretin-based OMM therapy. The key elements that emerged include the importance of preliminary patient education, the implementation of gradual and individualized dose escalation protocols, specific dietary and lifestyle recommendations for managing GI side effects, medical therapy, and the critical role of ongoing multidisciplinary follow-up care.
Preliminary education
HCPs suggest that setting expectations before starting incretin-based OMM treatment, preparing patients for potential GI symptoms, and offering management strategies may improve tolerance and adherence.
Most of the patients reported receiving relatively brief pre-treatment education from HCPs before starting the medication. This education primarily consists of reading a list of potential adverse effects, with short or no discussion on possible management strategies:
“The doctor read me a list of all the possible side effects of the medication and explained what is common and what is rare.” (Patient number #1).
One patient described receiving only a brief pre-treatment explanation from her physician, but, in contrast, gained extensive information from targeted social media groups:
“I would read the posts in the groups on social media as I like to be prepared. I knew what I was getting into and pretty much expected these side effects to occur.” (Patient number #6).
Given the substantial importance of preliminary education on treatment tolerance and adherence and its limited implementation in routine practice, Fig. 2 summarizes important key elements of pre-treatment education as identified by HCPs, as well as existing literature [21, 26, 28, 37]. These aspects should ideally be addressed by HCPs before medication initiation, or, if not possible, immediately after starting treatment.
Key elements of incretin-based obesity management medications pre-treatment education.
Gradual and tailored dose escalation
All HCPs indicated that gradual titration of incretin-based OMMs helps prevent GI side effects. Similarly, patients also mentioned a slower progression in drug titration, and in some cases, maintaining lower doses for extended periods as strategies to avoid GI side effects. These insights were particularly common among patients with prior experience in incretin-based OMM treatment. Another, but less common, alternative method of managing GI side effects that emerged from some patients and HCPs was switching to different types of incretin-based OMMs.
Despite preventive measures, GI side effects may occur, and they need to be managed.
Dietary and lifestyle recommendations for the management of GI side effects
As part of the focus groups with the HCPs, a comprehensive discussion was conducted regarding strategies for treating specific GI side effects during incretin-based OMMs treatment.
Table 3 summarizes recommendations for managing the most common GI side effects of incretin-based OMMs as arises by the HCPs and literature review [21, 26, 28, 38,39,40,41,42,43,44,45,46,47,48,49,50,51,52,53,54]. Recommendations from the literature were drawn from guidelines, reviews, and small-scale studies on nutritional management of GI symptoms related to various health conditions (e.g., gastroparesis, irritable bowel syndrome, and functional GI disorders).
Medical therapy to alleviate symptoms
Both patients and physicians report that the use of targeted pharmacological therapy is a common approach for managing GI side effects. These medications often aim to alleviate symptoms that are attributed, at least in part, to delayed gastric emptying or reduced GI motility.
Medications cited as being in frequent use are: Prokinetics (e.g., domperidone) or antiemetics (e.g., metoclopramide) for nausea, bismuth subsalicylate or pancreatic enzyme replacement therapy (e.g., pancrelipase) for diarrhea and abdominal discomfort, and osmotic laxatives (e.g., polyethylene glycol) or fiber supplements (e.g., wheat dextrin) for constipation. Heartburn and gastroesophageal reflux can be treated with antacids (e.g., calcium carbonate or magnesium hydroxide) or proton-pump inhibitors (e.g., omeprazole).
Multidisciplinary follow-up
Multidisciplinary follow-up, including a physician and dietitian, is a critical component of treatment success, as highlighted in HCPs’ focus groups. Effective communication between the patient and physician, including ongoing reporting of medication side effects, is essential to enhance treatment adherence and improve quality of life. One physician shared:
“Patients should contact me when side effects occur. You can’t overwhelm them upfront with every possible side effect and management strategy during one clinic visit – it’s too much information before they even start.” (Participant# 3, physician).
Nevertheless, in practice, most of the patients interviewed did not contact their physician when experiencing GI side effects. Some understood that these effects were related to the medication and believed that “this is the price you must pay.” While others initially did not attribute the GI symptoms to the medication. When speaking with their physician, patients found that the discussion was more likely to focus on dose adjustments to enhance medication effectiveness rather than addressing GI side effects.
Nutritional counseling by a registered dietitian is also essential alongside incretin-based OMMs to ensure balanced dietary intake and the prevention and management of GI adverse effects. One dietitian highlighted the increased risk of suboptimal food choices resulting from GI side effects:
“It influences their food selections, leading them to seek foods that are more gastro-compatible, which often translates to increased carbohydrate consumption.” (Participant# 6, dietitian).
Another dietitian emphasized the importance of maintaining nutritional follow-up throughout treatment:
“I see better side effect tolerance in patients who maintain regular nutritional follow-up.” (Participant# 5, dietitian)
link