,
by Raleigh McElvery, Neuro-Oncology Branch Scientific Communications Editor
Researchers share up-to-date trends in brain and spine tumor incidence, prevalence, and survival that incorporate new classification standards.
Recent technological advancements have provided unprecedented insights into tumor biology. This helps providers more accurately classify and diagnose tumors—potentially transforming personalized treatments and clinical practice.
Primary central nervous system (CNS) tumors are particularly difficult to diagnose because many are so rare. NCI-CONNECT’s mission is to better understand these tumors’ complex biology, in hopes of developing better approaches to care and treatment.
To further this goal, NCI-CONNECT partnered with the Central Brain Tumor Registry of the United States (CBTRUS) to capture the evolving definitions of 12 especially rare CNS tumor types. In a new study published in the Journal of Neuro-Oncology, NCI-CONNECT and CBTRUS share up-to-date patterns of incidence, prevalence, and survival for these select CNS tumors. Incidence is the number of newly diagnosed cases each year, while prevalence refers to how many people are living with the disease (regardless of when they were diagnosed). Survival is the number of patients alive for a certain period of time after their diagnosis.
This new study is a follow-on to a report published in 2019 by NCI-CONNECT and CBTRUS, which examined data on the same 12 CNS tumors spanning 2000-2014. The researchers hope their updated analyses will help the neuro-oncology community better understand the ever-changing definitions of these rare tumors, measure the impact of clinical care, and evaluate new therapies.
“Our CBTRUS database contains 20 years of data on every newly diagnosed brain tumor patient in the United States,” says Quinn Ostrom, Ph.D., the study’s co-senior author, co-principal investigator at CBTRUS, and an assistant professor of neurosurgery at the Duke University School of Medicine. “Our collaboration with NCI-CONNECT allows us to take these detailed data and characterize even the rarest tumors.”
These aren’t just numbers. They are game-changing insights with the power to affect patient care and outcomes.
Redefining Tumor Diagnoses
The study data came from the largest datasets available for characterizing brain tumor incidence and survival in the United States, collected by CBTRUS, NCI, and the Centers for Disease Control and Prevention. The incidence data spanned cases diagnosed from 2008 to 2019, while the survival data spanned cases diagnosed from 2001 to 2018. Prevalence was estimated as of December 31, 2019.
Importantly, these data included cases diagnosed using the 2007 and 2016 editions of the World Health Organization Classification of Tumors of the Central Nervous System (WHO-CNS). The WHO-CNS summarizes the World Health Organization’s current tumor classification system. Updates to these guidelines can have important implications for how providers diagnose tumors. While earlier WHO-CNS editions relied primarily on microscopic appearance to classify tumors, the 2016 version was the first to incorporate a tumor’s genetic characteristics as well. This impacted many of the 12 tumor types analyzed in the new study. Some were re-classified, renamed, or removed from the WHO-CNS altogether. In 2021, the WHO released another edition with additional changes.
Categorizing tumors based on detailed molecular features—in addition to appearance—is extremely useful, according to Byram Ozer, M.D., Ph.D., NCI-CONNECT assistant research physician and a co-author on the new study. “This ability helps clinicians better predict tumor activity, advise patients about treatment options, foresee potential complications, and adjust patients’ expectations,” he says. “From a researcher’s perspective, understanding the biological underpinnings of tumors provides clues about where tumors come from and how to develop more targeted therapeutics.”
Digging into the Data
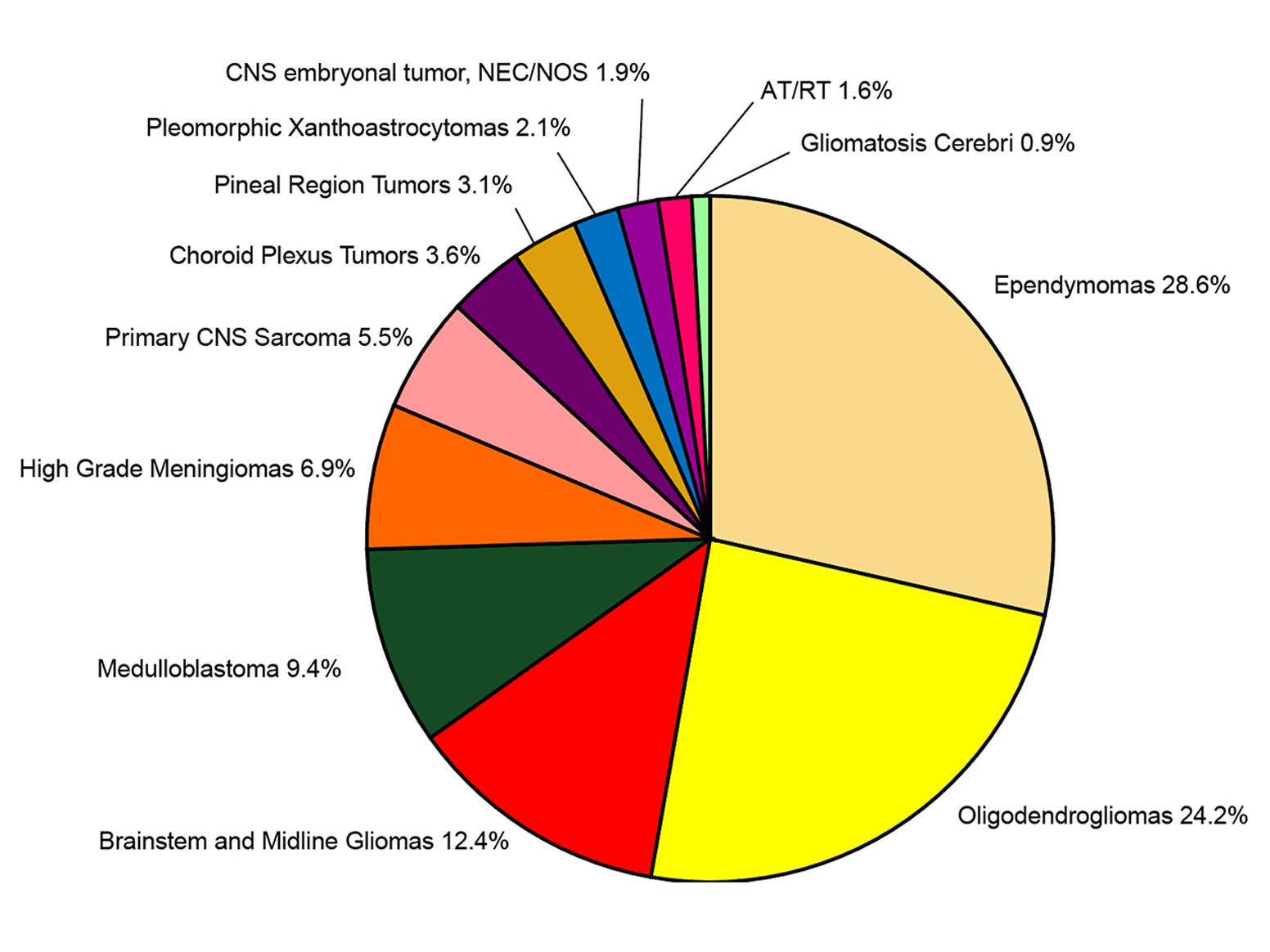
The researchers found that the 12 tumor types they analyzed accounted for about 5.3 percent of all primary brain and other CNS tumors diagnosed between 2015 to 2019. Most of these tumor types were more common in males, adults (ages 40 years and older) or children under 15 years old, and non-Hispanic white individuals.
Ependymomas had the highest incidence rate (1.47 per 100,000 people). They were also the most prevalent (19,320 cases as of December 31, 2019) and represented 1.6 percent of all brain and CNS tumors diagnosed between 2015 to 2019. Gliomatosis cerebri had the lowest incidence rate, likely because—in addition to being extremely rare—it was removed from the WHO-CNS 2016 edition.
Although the 2019 report focused solely on malignant CNS tumors (usually grades 2-4), the new, updated study also includes non-malignant tumors (those that are ungraded or grade 1). At the time of the previous report, there were not enough data on non-malignant tumors for the researchers to analyze. Today, they have finally amassed enough to draw definitive conclusions about these tumors.
“Including non-malignant tumors is key to calculating accurate prevalence estimates,” Dr. Ostrom says. “People with these tumors tend to survive longer, which means they form a large proportion of those currently living with such tumors. Prevalence estimates that exclude these tumors fail to account for a large part of the population.”
Of all the tumor types analyzed, ependymomas had the highest five-year survival rate (90.6 percent) of all the tumor types analyzed. Understanding statistics like these will allow providers to make informed decisions—and ensure cancer survivors have the services they need.
“The incidence, prevalence, and survival data presented in our new report will help inform the design of clinical trials and survivorship programs for people with rare CNS tumors,” says Marta Penas-Prado, M.D., NCI-CONNECT senior clinician and study co-author. In addition to driving clinical practice, these data will also help researchers plan additional studies to investigate the genetic and environmental causes of rare tumors.
From Trends to New Treatments
Overall, the trends in the new paper closely mirrored those reported in the initial 2019 study. The main difference was the prevalence, which increased for many of the tumor types—likely because the researchers also included non-malignant tumors in their new analyses.
“It’s both good and bad that the numbers haven’t changed much in recent years,” Dr. Ostrom says. “On one hand, it’s encouraging to see that incidence rates are not climbing. On the other hand, we were hoping to see improvements in survival rates. We anticipate that advancements in research will improve survival in the years to come.”
While the 12 CNS tumors analyzed are all quite rare, Dr. Ostrom estimates that there are about 4,600 people diagnosed with one of these tumors each year in the United States. “That means there are 4,600 people who could benefit from innovative clinical trials and supportive programs,” she says. “I hope our analyses underscore that this underserved population is important—and more than worthy of our attention and resources.”
link