We finally had 30 GC patients and 26 caregivers participating in the qualitative study. Of all participants, 5% were 18–34 years old, 7% were 35–44 years old, 30% were 45–54 years old, 36% were 55–64 years old, 20% were 65–74 years old, and only 2% were over 74 years old, with the largest number of patients between the ages of 55–64 years old (43%), and the largest number of caregivers between the ages of 45–54 years old (35%). 63% of the patients were male and 65% of the caregivers were female. The majority of patients (87%) and caregivers (92%) were married. 43% of patients with GC were in Stage I, 27% were in Stage II, 23% were in Stage III, and 7% were in Stage IV. 8% of caregivers were child caregivers, 31% were parent caregivers, 58% were spousal caregivers, and one (4%) caregiver cared for both his mother and spouse. Table 1 shows other demographic and disease related information.
Theme 1. Contextual factors
Contextual factors include the risk and protective factors that affect QOL of patients and caregivers and can be briefly summarized into three categories: (1) disease-specific factors; (2) physical and social environments; (3) individual and family characteristics.
Disease-specific factors
The disease-specific factors reported by the interviewees could be divided into three subcategories, including “the complexity and persistence of symptoms”, “impact of comorbidities”, and “occurrence of unexpected events”. Complex symptoms not only deteriorate the QoL of patients after GC surgery in the short term, but also some patients suffer from poor QoL in the long-term rehabilitation process due to the persistence and repeatability of symptoms. The existence of comorbidities further aggravates this dilemma, making patients bear a heavier physical and psychological burden. Despite the efforts of healthcare workers to reduce the incidence of adverse events, the inevitability of unexpected events still imposes additional psychological stress on patients and their caregivers.
The complexity and persistence of symptoms
Each interviewee reported being affected to varying degrees by a variety of physical and psychological symptoms. The most common physical symptoms in all patients undergoing radical gastrectomy were eating restriction (restriction of food intake and type), pain and fatigue, respectively. The most common physical symptoms mentioned by patients receiving chemotherapy/immunotherapy/targeted therapy were numbness, vomiting and loss of appetite. The most frequently reported psychological symptoms were anxiety, fear and shock, respectively. Almost all interviewees mentioned that patients had been troubled by multiple symptoms at one time.
“Uncomfortable when peeing, constant pain in my lower abdomen, the feeling of not being able to pee, just pain, it hurts when I pee. And shoulder pain, that is, it hurts when I enter this medicine into the IV infusion…When I can eat, my body starts to get better, and when I don’t eat, that dizziness…I can’t poop, (since the surgery) I haven’t pooped even once, that is, when I eat this [gruel], it is digested in one go. It hurts to urinate again, and there is no stool, eating soft is easily digested, there is no (stool).” “And…memory may be (not as good as before), I have to look at my cell phone for a long time in the past few days before I come back to my senses, it is definitely not as good as before, and it is definitely going to be even worse in the future if I have to undergo chemotherapy.” “I came for so many days only ate a little bit the day before yesterday, and before that for more than ten days, I only drank some water when I was hospitalized in the county hospital, and I didn’t even drink any water after I came here, so I only had fluids [nutrient solution]. Only in the last three days have I started to eat a little bit, before that I didn’t eat anything…I can’t eat anything I want to, when I want to eat they say you can’t eat so much, blah blah blah, it’ll have a bad effect” (P14).
One caregiver reported that the patient had barely slept for several nights due to the pain and that caring for the patient had disrupted his sleep pattern. “He slept fine last night…he hardly slept the night of the 16th 17th and 18th…on the night of the 18th he was in a lot of pain…and then he was up all night with his eyes open…the IV that was put in last night made me not sleep much either” (C21). The patient also reported other symptoms: “(With the drain inserted) it’s like there’s something going through the stomach, it’s a little swollen and painful when I move and turn over, it feels as if there’s something hard in there, and there’s a feeling of a foreign body. Coughing makes the whole piece [abdomen] ache. The waist here, it gets sore after sleeping too much…the strength is much better than before, I remember the first time I got out of bed there was no strength at all, no strength at all” (P21).
Due to the long chemotherapy cycle, the patient experienced discomfort symptoms again and again, which lasted for about a week after chemotherapy and slowly subsided. One patient described the symptoms he experienced after chemotherapy: “Weakness in my limbs, I don’t want to eat…It takes a week after this chemo to slowly feel better. I still want to vomit, but I can’t vomit anything. I can walk, but when I walk, I don’t have the strength, I can’t walk for a long time, and I feel a little bit better after one week after the chemotherapy” (P30). He repeatedly mentioned that these uncomfortable symptoms did not gradually improve until about a week after chemotherapy, but he would have to follow up with several more chemotherapy sessions in the hospital, and the thought of this almost broke his spirit. “Every time I come for chemotherapy, I have a headache and sweat, I’m afraid to come for chemotherapy, as soon as I step my foot through the door of the hospital I feel sick, it’s so hard, it’s so hard” (P30). A patient with four years’ experience of chemotherapy had the same distress; the cumulative effect of the long-term treatment had conditioned him to the infusion needle, and he felt scared at the sight of it. “I’m really scared (of needles), do you know how many needles I’ve had in four years, intramuscular injections, intravenous infusions, and now I’m just like a child, I’m a little bit scared when I see a needle, and it hurts so much to get a shot” (P28). Another patient who underwent chemotherapy described the severity of the loss of appetite: “When I got home, I had no appetite for food and I couldn’t eat, and I lost 2–3 pounds for every chemotherapy session, and I’ve lost more than 30 pounds in total so far. I was 150 pounds before I had the surgery and now I am less than 110 pounds” (P17).
Impact of comorbidities
Seven of the thirty patients interviewed had two or more diseases, and one patient had a postoperative complication [gastroparesis]. Comorbidities often mean that patients need to manage multiple conditions at the same time, which not only requires strict adherence to a multi-drug regimen, but may also face shuttling between different healthcare facilities for care, increasing the complexity of treatment for patients and thus reducing their QoL.
“I suffer from lumbar disc herniation, for which I have had many x-rays and I take a lot of medicine” (P7). “She spent a lot of money now on herniated lumbar disc, she went to Guangzhou, Shenzhen, and then she took a lot of medication, treatment here and there, and in the end it was not cured, (it’s been) cured for years” (C7).
“He had a skin disease before and it would itch on his body…he was hospitalized 4 times in the Provincial Skin Hospital, and then later, he had a relapse (of the skin disease) 1 month later, and he went to be hospitalized again after the relapse” (C24). “Whenever I smoke my skin itches, the itching is maddening…the doctor also said that you can’t cure this skin disease, after a while it will come back again” (P24).
Comorbidities may also increase the risk of disability and death, especially in the elderly population. A caregiver of a GC patient who was receiving chemotherapy described the patient’s comorbidity in detail: “For the first month after the operation [radical gastrectomy], the place where (he) pulled urine [urethra] was very painful, and he could not pee. He went to the county hospital for treatment for more than a week, and then he came here for chemotherapy…(The doctor) said he had some kind of urethritis, an inflamed urethra. He fell off a mountain many years ago, broke his head, had an operation, and that memory is not good. He often gets dizzy, falls to the ground like a fall, he does not have any consciousness, this situation has happened several times, like a sequelae, falls to no consciousness, wait for half an hour or an hour will wake up, wake up to know that fell to the ground…I’ve been taking care of him for more than half a year.” (C10).
Occurrence of unexpected events
Unexpected events are sometimes difficult to avoid during treatment, and these situations may cause patients and caregivers to feel deep guilt and self-blame. They may worry that their negligence has caused unnecessary trouble to the health care team or even that the health care provider will be upset or angry. This emotional burden can sometimes lead to additional psychological stress for patients and caregivers. This pressure can lead them to take extreme or drastic actions in response to the accident, in an attempt to ease their feelings of guilt or to try to compensate for the impact.
“Last night here…At night, the area [wound gauze] itched a little hard to sleep, and when I fell asleep, I accidentally dropped all the gauze wrapped in it. The nurse came round in the evening and said, ‘Ouch, how did you drop the gauze and’ called the doctor on duty “(P24).
“Did he accidentally drop the gauze last night, which made the doctor angry? Maybe it was the gauze that was not attached properly when the dressing was changed. I tied up his hands today, I can’t do without it, he wants to catch it again” (C24).
Physical and social environments
Physical and social environmental factors are external conditions that affect the QoL and health behaviors of individuals and groups. According to the interview results, the physical or social environmental factors could be summarized into four subcategories: “quantity and quality of medical resources”, “difficulty in certifying social assistance and complexity of the process: related to social networks”, “economic status and life pressure”, and “affected by external environment”. The quantity and quality of medical resources directly affect the continuity and effect of treatment for patients with GC, and the lack of resources may lead to the interruption or delay of treatment. The difficulty of social assistance certification and the complex processing process may hinder the families of GC patients from getting financial assistance in time. The interviewees believed that the support degree of social network played a key role in this process. Economic status and life pressure are important factors affecting the psychological and material well-being of patients and their caregivers. Financial difficulties can further aggravate life pressure and affect the QoL. External environmental factors, such as ward noise and the evaluation of others, may interfere with the recovery and rest of patients and their caregivers and affect their mood as a result. These factors interact with each other to affect the short-term and even long-term QoL of GC patients and their caregivers.
Quantity and quality of medical resources
In China, high-quality medical resources are mainly concentrated in provincial capitals, leading to a widespread public belief that if you have a “terminal illness”, you can only travel to the provincial capital city to be “rescued”. That view has triggered a flood of patients to the provincial capitals, sometimes overstretching their health care systems to the brink of collapse. The resulting chain reaction, including the extreme shortage of hospital beds and the common phenomenon of “one bed is hard to find”, further exacerbating the contradiction between supply and demand of medical resources.
“That’s what the doctors in the county said, that I’d better come to the best hospital, and I don’t know how I got so sick. The doctors are saying that I had better come to a big, good hospital for this operation” (P7).
“Now I have a bed when I come” (P10). “When we used to come (to the hospital) there were no beds, no beds, we stayed out for several nights” (C10). “In the morning there were a lot of patients to wait for infusion, there was no way, now (this situation) is a little bit better.” (P10).
Some interviewees do not trust the medical technology of local hospitals, and they believe that if they are treated in local hospitals, they will only face “death” in the end. “If you get treatment at the county people’s hospital, you will definitely die, and he [the doctor] said he would use intravenous drips. Can this save lives? The situation was so serious that I vomited blood (from my mouth)” (P28).
In fact, after the onset of symptoms, some of the patients were first examined in local hospitals, but the initial under-diagnosis by the doctors led to the deterioration of the patients’ conditions. One interviewee described how general practitioners misinterpreted patients’ symptoms and treated them until their condition worsened. “When she started to lose weight, I took her to the hospital for two checkups which showed normal results. She didn’t have a gastroscopy at the time, the doctor didn’t even suggest we get one, all the other tests were done. Then it started to get worse, she couldn’t eat anything, and when she did,she vomited, and when we got to the hospital we asked for a gastroscopy ourselves, and that doctor hadn’t even suggested that we get a gastroscopy yet, and it was really pissing me off!” (C26).
Difficulty in certifying social assistance and complexity of the process: related to social networks
Families with GC commonly face both psychological and physical challenges. In the absence of adequate health insurance support, the expensive cost of surgery significantly adds to their financial pressure. Faced with such a predicament, they often turn to the social assistance system to maintain their basic living needs. However, accessing such assistance is not easy due to limited social assistance resources and strict eligibility criteria. Many interviewees expressed their concerns during the interviews.
“I plan to go home this time and ask them [township government staff] to help me apply for subsistence allowance, but I don’t think I can get it without any relationships. It’s difficult to get subsistence allowance in the countryside without relationships. To apply for subsistence allowance in the countryside you have to have a relationship with the government staff…without that, they won’t even pay attention to you” (C11).
Interviewees pointed out in their interviews that the procedures they faced in carrying out the preparation and submission of qualification materials were extremely complex. They had to repeatedly go back and forth between different departments in order to complete the necessary formalities. “It’s not like I know any official, so it took a long time to sign and stamp and find this and that” (P2). The fragmentation that exists between the healthcare system and local policies not only makes it more difficult for applicants to prepare materials, but may also lead to delays in applying for assistance, thus affecting the timely access of people in need to necessary social support. “We are self-funded, and some people go to the local government as if they can still be reimbursed a little bit for treatment, and I need a certificate, and I don’t know where to get it. I asked the staff there [township office] and he told me to find the doctor in the hospital to fill out this form…Then I asked the doctor and the doctor said he didn’t know and I didn’t know how this was going to be done” (C10).
Economic status and life pressure
Almost all of the interviewees in the study conducted had financial difficulties. High medical costs (some patients were treated for multiple illnesses), expensive medication costs, deterioration of the family’s financial situation, and unemployment all disrupted the original rhythm of these families’ lives and exacerbated their financial stress. These financial burdens not only affect the patient’s ability to obtain continuous medical care, but also have a negative impact on the QoL of family members.
“Our family has no financial resources anymore, we rely on me to work, and he can’t work anymore, it’s all on me to work alone, my daughter needs tuition fee of 50,000 RMB (about 7,050 US dollars) per year to go to university for four years, his little bit of retired salary is surely not enough to cover the expenses, there will be times when we have difficulties in terms of finances, and this time, he was hospitalized, and he spent all the family’s money on the medical treatment, almost spending more than 58,000 RMB (about 8,178 USD)” (C21).
“Mostly it’s about imported medicine. This medicine is not covered by medical insurance… in terms of the economic pressure, we had to pay out-of-pocket more than 100,000 RMB (over 13,000 USD). After the surgery and the insurance covered some costs, we still had to pay about 70,000 RMB (nearly 10,000 USD), plus there are other living expenses. I’ve been here with him for more than ten days, and I can’t earn money either” (C3).
The ongoing financial pressure from cyclical chemotherapy cannot be ignored. “(QoL) is definitely far worse compared to what it was before, it’s definitely worse, he still needs money (for treatment), he still needs post-treatment, right? It’s always going to cost money because he’s got a family to support and he’s got no financial income” (C2). Patients further elaborated that due to the lack of a stable financial income, they experience challenges in borrowing money as potential creditors may be skeptical of the borrower’s ability to repay the debt, making it difficult for patients and their families to obtain the necessary financial assistance. “Let’s not talk about anything else, let’s talk about a simple one, that is, I have this disease now, it’s not easy to borrow money from people, it is very realistic, who will lend you [money] if you don’t have [financial] resources, what are you going to pay it back with? It’s just like that” (P2). Another interviewed patient faced even more severe financial pressures, with his medical expenses mainly financed through a bank loan, on top of which the patient had taken on a huge debt. “I still owe 180,000 RMB (about 25,380 USD), I borrowed about 100,000 RMB (about 14,100 USD) (for the treatment) of this disease, and I borrowed about 100,000 RMB before that, and my son’s education is all on loan, and all of it was borrowed from the bank” (P17).
A diagnosis of GC poses an additional burden on families already in financial distress. One patient’s spouse was unable to perform heavy labor due to activity restrictions following cardiac stent implantation, and the patient himself was unable to continue working due to the demands of treatment for GC. This situation exacerbated the family’s financial stress and created uncertainty about future QoL and financial security, leading the patient to feel confused about the family’s future livelihood. “Because my husband’s health is not good either, he also had a stent in 2008, he has a bad heart, high blood lipids, he also had an operation, so at that time I got this disease I really kind of can’t bear it, because my husband can’t do heavy work, plus I don’t know exactly (when I will get well) with this disease now…” (P19). One caregiver reflected on the significant reduction in their employment opportunities due to age-related restrictions, which had increased the stress of living in their household. “I’m getting older now, no one needs me when I go to do odd jobs, people are afraid to accept me and I’m stressed” (C11).
Of all the interviewees, only one dyad did not suffer the negative effects of financial stress because they had higher pensions and better living conditions, which was enough to cover any medical expenses. “We have been retired for ten years, and to tell the truth, my retirement salary is very high, and the retirement salary of the two of us is almost 10,000 RMB (about 1,410 USD) a month, and we usually don’t spend that much” (P24).
Affected by external environment
The healthcare environment, especially the ward environment, has a significant impact on the QoL of hospitalized patients and their caregivers. In multi-occupancy wards, differences in the living habits of patients and their caregivers may lead to mutual dissatisfaction and conflict. Such environmental factors may adversely affect patients’ psychological state, emotional stability, and therapeutic outcomes, thereby reducing the overall QoL during hospitalization.
“Didn’t sleep well for the first two nights, the ward was so noisy, a few people snoring so loudly, playing with their cell phones with the sound out loud and not turning it down” (P16).
“There was a man who was so grumpy before, we told him to turn down the sound on his cell phone and he didn’t even listen, he stayed here for two days” (C16).
Another interviewee noted that she had to suspend her personal hobbies due to patient care responsibilities. The main motivation behind her decision-making was the concern about being judged or blamed by others, which could lead to psychosocial stress and affect her willingness and frequency of participation in personal hobby activities. “I used to go to dances, but now I don’t go, I’m not in the mood to go now, especially our rural people, they love to gossip” (C2).
The living environment is one of the many key determinants of QoL, and it includes elements such as proximity to natural green spaces, convenient park facilities, and ease of pet ownership. One patient was convinced that a quality living environment could significantly improve the overall quality of his life: “Take a walk I do, I don’t go for walks now that it’s cold, but when it’s hot I go to Tianhu Park in the morning, take my puppy, walk with my puppy, I have a pretty good QoL” (P24).
Individual and family characteristics
Individual and family characteristics encompass a wide range of attributes, including the physical, psychological, social and economic characteristics of the individual, as well as the structure, functions, resources and support systems of the family. Based on the interview results, individual and family characteristics can be summarized into three subcategories: “patient disobedience”, “burden of family responsibilities”, and “patient-caregiver QoL interactions: related to caregiver identity”. GC patients’ disobedient behavior may stem from a lack of knowledge about the disease or resistance to treatment, which not only affects treatment outcomes but also increases the psychological burden on caregivers. The burden of family responsibilities, such as raising children and supporting the elderly, is also a constant stress for GC patients and their caregivers, especially when they themselves are facing health challenges. In addition, the QoL of patients and caregivers is mutually reinforcing, with caregiver identity often determining their roles and responsibilities within the family, which in turn affects their emotional state and coping strategies.
Patient disobedience
Caregivers play the role of monitoring the daily behavior of patients while performing their caregiving duties. Out of a sense of concern and responsibility, caregivers will intervene promptly when a patient with GC does something that is not conducive to recovery. However, in some cases, the patient may ignore the caregiver’s advice and treat it as an unnecessary intervention or not pay attention to it, resulting in the caregiver feeling helpless.
“He once after chemotherapy here, (at that time) his body was very good [had recovered well]. One day after dinner he couldn’t stay idle, went out to the mountains to cut wood, and when he came back (his body) was not good, and the next day he was lying in bed and couldn’t get up. Then he asked me to take him to the hospital, got an infusion, and then went to a big hospital on the third day. You can’t work, and the doctor explained that you don’t have to work, you have to rest more. But he couldn’t stay idle, he had to go to work, and when he did work, his body didn’t work” (C10).
“Diet-wise sometimes she doesn’t listen to my advice, she’s kind of self-centered kind of [doesn’t listen to advice], sometimes kind of self-absorbed. Her friends are all in school, she only goes out once or twice in a long time, and most of the time she is at home. When I ask her to go outside for a walk, she says that the weather is so cold and she doesn’t have much energy. I don’t dare to say too much, if I do, she will get angry” (C25).
A interviewed dyad had an argument during the course of the interview due to a difference in perceptions.
“He usually doesn’t listen to me” (C2).
“There would have been no need to listen too much to women” (P2).
“You can’t eat certain foods, you don’t listen when I say so, you get angry when I get angry, I see you eating something you can’t eat and I’m afraid that it’s not good for your health” (C2).
“That’s what the doctor said, I can eat anything as long as I don’t feel sick to my stomach if you eat it, just eat a little bit less. I was already eating very little, and she told me not to eat any of those, so how can I have strength if I don’t eat them” (P2).
“I can’t eat cold fruits, but I have to steam them and eat them warm, is it troublesome?” (P2).
Burden of family responsibilities
Traditionally, men are considered to be the “head of the family”, responsible for taking care of their spouses and family members, as well as the spiritual pillar of the family. Men are given specific family responsibilities and expectations. Therefore, when a male member of the family suffers a major health crisis, such as GC, his spouse may feel great psychological pressure and insecurity. “Everything was defeated by the economy, defeated by his health right? Before life are still living average, now…alas, the head of the family, compared to before, now (QoL) is definitely worse” (C2).
Not only that, the interviewees were faced with unfulfilled family responsibilities, including child rearing and parental support, and the unfulfillment of these responsibilities caused intense conflict and a deep sense of guilt within them. “I definitely wish I could live a few more years on my own because I have a heavy burden with parents to support and children to raise. My youngest son is 10 years old and in fourth grade, I’m in my 50 s and my wife is 41. If I can live a few more years, raise my son to adulthood, take care of my parents, and bring these things to a successful conclusion, that would be my ideal life. Now that I haven’t accomplished my basic responsibilities, I feel like my life isn’t complete and I’m too sorry for my mom and dad.” (P28).
Patient-caregiver QoL interactions: related to caregiver identity
In the interview data collected, the vast majority of interviewees noted that there was an interaction between the QoL of GC patients and their caregivers, a phenomenon that was particularly pronounced in the case of spouses and parents as caregivers. Part of the spousal caregiver group expressed the view that, although their children had created their own families, their own social support networks were largely dependent on their partners. As a result, they felt that they could face a significant lack of social connection in the event of losing their partner, a concern that highlights the centrality of spousal relationships in later life and their importance to an individual’s sense of emotional security. “If he’s gone I’ve lost everything, son he’s got his own family” (C15).
Similarly, parental caregivers felt that they were too old to help their children through difficult times, resulting in deep feelings of self-blame and powerlessness. “Me, I’m not very educated, I’m just doing menial work, and in my mind I just want to earn some money and help my son, that now I’m old, I can’t help much” (C5). They believed that only when their children’s health was restored could their QoL be realized in the true sense. “How can that have no effect, my son’s health is good, we as parents (QoL) will be really good” (C5).
However, adult–child caregivers had a different view when confronted with this issue, as they had unimpeded access to information about the disease and therefore did not encounter any problems in caring for their patients, and even when they did they were always able to solve them in a timely manner. Based on these factors, they felt that their QoL did not suffer any negative impacts due to the hospitalization of their patients. One caregiver of a child who was attending her senior year of college said, “Now that I’m in my senior year, it’s okay, it doesn’t really affect my life” (C17).
Theme 2. Knowledge and belief factors
Knowledge and beliefs are real information and perceptions about health status or health behaviors. Based on the results of the interviews, knowledge and belief factors can be summarized into three categories: “self symptom assessment and healthcare seeking behavior: lack of health awareness and professional knowledge”, “health information delivery and accessibility” and “life priority adjustment: influenced by health beliefs”. These categories reveal the influence of knowledge and beliefs on the health behaviors of GC patients, and by increasing the health awareness of GC families, optimizing access to health information, and guiding patients to develop positive health perceptions, it is possible to promote more effective health behavior change and improve their QoL.
Self symptom assessment and healthcare seeking behavior: lack of health awareness and professional knowledge
Due to the lack of appropriate professional knowledge, it is difficult for GC patients to judge what causes the discomfort when they are confronted with it. In most cases, patients do not consider a little bit of stomach discomfort symptoms worth being taken seriously. “Before she was uncomfortable…at first she thought she didn’t have a serious problem, so she wondered if she had eaten too much at night, and then in the second half of the night, her stomach became even more uncomfortable. The discomfort lasted about a month and the weight slowly went down” (C26). Some patients did not realize the severity of the situation until they experienced severe vomiting of blood and black stools, which largely contributed to the delay in seeking medical attention.
“It was just as early as ten days or so ago, probably last month at the construction site, and all of a sudden I had black stools for five or six days, and then I went straight to our township hospital for several intravenous drips, and that doctor suggested that I go to the county hospital to see what’s wrong with this stomach” (P14).
“Before, I would vomit blood, spit blood…spit a big, big bowl of blood” (P8).
In exploring the causes of GC, patients interviewed generally cited poor dietary habits, smoking and alcohol consumption as the main risk factors for developing GC. In addition, self-reflection on lifestyle and health status also identified drug use, mood swings, overwork, and progression of chronic diseases as factors that may contribute to the development of GC. One patient had a misperception of the cause of GC, believing that her particular preference could lead to GC: “Is it because I like to bite these meats in my mouth, bite and like to swallow, is it because of that” (P18). Another patient reported no bad habits and did not become aware of a potential health problem until she experienced recurring symptoms of stomach discomfort. During the onset of symptoms, she took treatment measures that consisted solely of purchasing medications, and she suspected that these symptoms could be related to the long-term effects of COVID-19 infection. “All three meals were relatively regular, and since COVID-19 infection she started having stomach pains, almost a year ago, and she’s had stomach pains on and off for almost a year. She said that when she was infected her stomach was uncomfortable off and on, and when she was uncomfortable she went to the doctor to get some anti-inflammatory pain medication, and when she took the medication she felt better, and when she got better she didn’t worry about it, and then she went to have a gastroscopy after it got worse and worse, and that’s when she found out about this [GC]” (C23).
The lack of health knowledge among patients or caregivers is very likely to lead to neglect of the severity of the condition, as they subconsciously believe it is not a serious problem. This phenomenon is common in rural areas or underdeveloped regions of China. Such disparities in health knowledge, caused by lack of access to professional health education, can also lead to excessive reliance on professionals during decision-making processes, inability to recognize dangerous symptoms, and ultimately result in severe consequences.
One interviewee said that rural dwellers rarely go for proactive screening for GC, which may be a reflection of the low awareness of proactive screening among rural dwellers. “It can’t be detected without screening, and very few of us in the rural areas would go for this kind of medical checkup” (C18). Among all the respondents, only one patient would take the initiative to have regular screening for GC: “Since I found out that I have gastric disease, I have been having gastroscopy every year since 2018…Before that I had atrophic gastritis, chronic atrophic gastritis…I searched on the internet that chronic atrophic gastritis is a pre-cancerous lesion well…I just have regular gastroscopy, I can’t not have regular gastroscopy, otherwise the condition will be more serious” (P22).
Health information delivery and accessibility
Not being able to use electronic devices, age, living in a rural area, and literacy level are all important influencing factors that affect the delivery and accessibility of health information. These factors affect communication between GC patients and their caregivers and professionals, which in turn hinders their ability to accurately understand and effectively receive information related to GC.
“I don’t know how to use my cell phone, so I go and ask my child about this disease, and my child will ask the doctor and nurse if he doesn’t understand” (P3).
“If the young people are not here, the old people don’t understand anything, right? Speaking to the young people they can understand (it is easy to communicate when doctors talk to the young people), the old people don’t understand anything, I haven’t read any books, I don’t understand anything” (P7).
Caregivers believe that disclosure of diagnostic information may be emotionally disruptive and trigger emotional distress or depression in patients, especially in older patients or those with AGC. In clinical practice, this approach often results in patients being kept in the dark about their true condition, or being informed about their health status only at later stages of treatment, on the grounds that the emotional and cognitive state of the patient may affect his or her ability to learn and adapt during the treatment process. However, patients felt that they had the right to know about their condition, despite the fact that individual patients were in the advanced stages of GC. They advocated that knowledge of the condition was essential for developing strategies to cope with the disease, helping to reduce anxiety and fear due to uncertainty, thus granting patients a greater sense of control and participation in treatment decisions.
“It doesn’t matter, because I’m a person who doesn’t care, those doctors don’t tell me (my condition), I say don’t be afraid…I say this is definitely cancer, it’s an early or late stage thing, it’s not possible to not have it…I already know…I’m not afraid of it, I’m not afraid of it, I can’t be afraid of it, how can I am afraid of it?” (P6).
“My husband also did not tell me, then I saw the medical record called what malignant tumor. I asked the doctor, I said that this disease is divided into early, intermediate and late stages, I asked him I was…what degree, he said don’t worry has been done after surgery, I am now still a little worried in my heart. I asked my husband that day, because my character is also more impatient, as if I know would be better, I said you tell me if I am advanced, he said no, anyway, I saw that medical record written above quite serious” (P19).
Some patients reported that communication with healthcare professionals was often limited, with doctors usually responding only to questions posed and not offering to provide additional health guidance information. “Doctors and nurses, he/she answers whatever you ask, if you don’t ask he/she doesn’t answer, if you ask a little bit he/she answers a little bit” (C4). Frequent questioning of the doctor when the patient wants further information shows that it is unwise because the doctor is busy and has limited free time. “(Communication with the healthcare provider) is also rare because I…he doesn’t have time either” (P5). Inadequate communication may lead to impaired motivation of GC patients and their caregivers, which in turn affects their initiative, autonomy and participation in the treatment decision-making process.
In terms of access to medical information, some patients and caregivers preferred to proactively utilize online resources in order to search for health management information related to their illnesses in order to fill information gaps in their medical consultations. Among these participants, dietary care during postoperative recovery was a top concern. In addition, they also gained first-hand experience and professional advice through interaction with patients, healthcare professionals, or friends and relatives. “I would go and search for some information about this disease, such as what I can eat and what I can’t eat, I would search for it, and I would also communicate with my fellow patients, it’s human nature. What I don’t know I will also ask them [healthcare workers] and they will also give me careful answers” (P2). Another caregiver did not know how to use the Internet, so she obtained relevant information by buying paper books: “I have bought several books on stomach care at home and two books on GC” (C25). Only one caregiver, who had a background in the medical profession herself, did not encounter barriers in obtaining information about the disease and communicating with medical professionals: “I studied this profession [medicine] before, my brother also studied medicine, I do know this [GC], and I told the doctor you just have to tell me about the surgical plan and the risks. The doctor said there is no barrier to communicate with me” (C1).
Life priority adjustment: influenced by health beliefs
Individuals hold different perceptions of health in different physical health conditions. During the self-perceived stage of being in good health, minor physical discomfort tends to go unappreciated, as individuals may prioritize work and financial gain. However, when faced with serious health challenges, individuals’ health perceptions may shift, when they tend to recognize the primary value of physical health, realizing that neither wealth nor social status can lead to substantial QoL in the absence of a healthy body. This shift highlights the dynamic relationship between health perceptions and an individual’s health status, and how the place of health in an individual’s value system may be reassessed as health status changes.
“As soon as I feel sick I go to the hospital immediately and he [the patient] says that I take medication all day long and if I don’t take medication I don’t feel well, instead he says this about me, he doesn’t see the doctor in time but he says this about me, so he gets into this situation” (C21).
This patient now sees the loss of his health as a loss of value in his lack of existence: “It’s nothing like it used to be when I was well, it’s nothing like that. I used to be able to walk around, now I just sleep here, like a person of no use” (P21).
After experiencing the major health crisis of GC, the interviewees generally engaged in profound self-reflection, and their perceptions shifted as they began to view their health as their most valuable asset. In their narratives, a healthy body became the cornerstone of QoL, while they showed relative indifference to other aspects of life, such as material wealth and social status.
“No way, work and other things have to be put aside, health is the most important thing. Good health is the greatest happiness. A person, you say, if the body is not healthy, have more things are useless. It’s good to be able to eat, sleep, earn, play, and feel tired, and it’s useless to have a lot of money when you’re lying in this place [hospital]” (C18).
Theme 3. Self-regulation factors
Self-regulation is an iterative process in which people engage in order to change health behaviors, which can be briefly summarized in this study under two categories: “strategies for health behavior change” and “role adaptation and emotion regulation.”
Strategies for health behavior change
When faced with the major stressful event of GC, some interviewees demonstrated positive coping strategies, such as changing unhealthy lifestyles and engaging in appropriate physical activity. These decision-making strategies reflected their proactive approach to disease management and active participation in treatment. They tended to adopt measures that were considered beneficial in the fight against cancer and demonstrated confidence in overcoming the disease, reflecting the importance of self-management.
“Now I just want to get better quickly so I just exercise everyday like climbing stairs” (P19).
“I just listen to music and take a walk, something like that, to relax my mood a bit, I’m almost at retirement age anyway” (P22).
“In this condition now, I will definitely pay more attention to their habits and review, and I will never let them eat what they can’t” (C26).
However, when patients are unable to accept a sudden cancer diagnosis, they may adopt some negative coping mechanisms. In this case, some patients may develop a pessimistic attitude towards life, believing that being diagnosed with GC means the end of their QoL, thus adopting a negative and aimless belief in life. “It can’t improve (QoL), it’s still the same way to live, living through one day to the next” (P12). Another patient who was undergoing chemotherapy, due to the severe challenges of her family’s financial situation, generated the idea of abandoning the treatment: “It’s just that this medicine is too expensive, I don’t even want to come this time, my son asked me to come, I don’t have enough money for the treatment, it’s not like I just need to have the treatment once or twice. If you don’t have money it is better not to see a doctor, just go to the land [implying death]” (P3).
Some interviewees tended to cope independently with the challenges posed by a cancer diagnosis, rejecting outside assistance and even choosing to suffer in silence in the face of physical discomfort and emotional distress. Such behavior was motivated by consideration for their caregivers or family members in order to avoid causing them additional worry and stress, and embodied a spirit of self-sacrifice to protect the interests of others.
“Any difficulties have to be put into the heart and not spoken. Even if there is too much pressure, everything needs to be faced by oneself” (C5).
The assistance of others in times of hardship is sometimes seen as a debt of gratitude, an intangible social debt that is difficult to quantify and repay. This debt is often accompanied by emotional and moral obligations, and its repayment may not be limited to the material level. As a result, some cancer families may refuse help from others to avoid not being able to repay such a debt of gratitude. “I don’t need this help, I’m afraid I can’t pay back the favor” (P20). Some patients chose to face their difficulties alone with the idea of not wanting to bother others: “Other people use the Waterdrop Medical Crowdfunding software to raise money [a social fundraising application], but I never do it, I just think I can’t bother other people, and try to solve the problem by myself as much as I can, right? That’s the way I am, I have different personal ideas, I try to solve the problem by myself” (P28).
In contrast to coping alone, some patients were reluctant to self-manage after surgery, and their lives were highly dependent on the care of their families: “My wife is very diligent and takes care of me, she buys everything from the countryside or grows it herself [organic food], and she is in charge of all the meals and household chores” (P28).
Role adaptation and emotion regulation
GC patients who are faced with the transition from a healthy to a diseased state often have difficulty adapting quickly to this new identity. This maladaptation leads to a strong desire to be discharged from the hospital, which serves as a psychological mechanism to deny their reality as “patients”.
“I had to face reality, I had to accept (the change in the role of patient)” (P2).
“I am ready to be discharged tomorrow…I feel like I’ve fully recovered, but the doctor won’t let me go, saying they need to observe me for another two days. If I can be discharged, let me know as early as possible” (P24).
After the diagnosis of GC, patients and their family members often go through a series of complex stages of psychological adaptation. They are first shocked and suspect a misdiagnosis: “At first we all wondered if there was something wrong with this diagnosis” (C25). They lamented the injustice of fate: “Sometimes I wondered why it was so unfair, she was still so young” (C25). They were also very scared in the face of the unknown cancer: “As soon as I heard [the news] I was cold from my feet to my head, I was shaking all over, the local doctor said it was cancer” (P19). One patient was very regretful about his past alcoholism and could have avoided the misfortune of GC if not for his chronic drinking: “I bought 20 pounds of alcohol a month ago, it was that 20 pounds of alcohol that almost killed me, every day I came home from work and had a sip after a sip and that’s it, it was that 20 pounds of alcohol that caused the black stools” (P14). Another interviewee felt very grateful to have caught the cancer earlier: “Luckily it was because of the stomach pains that she found out about the cancer, otherwise we don’t even know how long it would have taken to find out” (C18). Cancer families also felt worried and anxious about the uncertainty of the future: “I’ve had the operation I’m still…anyway I’ve been thinking about it, GC has cost me so much money and I’ve suffered so much, and I’m not sure if it’s going to get better, if it’s advanced or not, and just worrying about it all the time” ( P19). Even they may develop despair: “As soon as I hear that it is cancer then I think it is…hopeless” (P19). Eventually, most of the interviewees accepted the reality through continuous self-adjustment: “At first he couldn’t accept it, then slowly he accepted it. He said, ‘Opps, whatever, I’m so old anyway, everyone else younger than me has passed away’.” (C10). They tended to accept the fatalistic view that the fate of individuals was governed by supernatural forces, and therefore they chose to follow the will of God, adopting a passive attitude and a deep sense of powerlessness towards such a major event as cancer: “There’s nothing I can do about it, if God doesn’t want me to live, I can’t live, there’s nothing I can do about it” (P14).
The connotation of “being a mother is being strong” is illustrated by a mother caregiver who struggles to restrain herself in front of her child: “We don’t even dare to cry in front of her, we always hold it in [bitter smile]. I’m okay, I can control it, I can’t be weak in front of her, I have to be strong!” (C25). One patient struggled to manage her emotions effectively due to her deep fear of cancer: “I can’t regulate my emotions, I’m scared to death, how can I regulate [my emotions]” (P18). However, some of the interviewees held a positive attitude, believing that even in the face of the challenges of GC, they were able to cope with most of life’s difficulties by maintaining a positive mindset. “It’s okay, mentality…must have a good mentality, a good mentality can solve most of the difficulties” (C24).
Theme 4. Social facilitators
Social facilitation occurs in interpersonal relationships and can be facilitated by family, friends, or even societal forces that assist or promote an individual’s or family’s participation in health behaviors. In this study, social facilitators can be categorized into the following three categories: “positive motivation and emotional support from family, friends, and society” “missing companionship and challenges encountered by family and friends visiting the patient after surgery” and “caregiving burdens and challenges”. Specifically, positive motivation and emotional support from family, friends, and society can significantly enhance patients’ treatment adherence and motivation to recover, and reduce the psychological stress caused by the disease. However, when companionship is absent, such as when family and friends find it difficult to visit patients for various reasons, patients may feel lonely and abandoned, which not only affects their recovery process, but may also have a negative impact on their long-term QoL. In addition, the burden of caregiving may also cause both physical and psychological stress to the caregiver, and these stresses, if not properly managed, may lead to health problems for the caregiver himself or herself, which in turn may affect the functioning and well-being of the family as a whole. The role of social facilitation therefore plays a crucial role in providing support and mitigating these challenges.
Positive motivation and emotional support from family, friends, and society
In the face of the negative emotions experienced by GC patients or their caregivers, positivity motivation and emotional support provided by family, friends and the community play a crucial role. Such support can provide positive psychological cues to patients and caregivers, especially during the period when they feel that their lives are limited, and positive encouragement and emotional support can rekindle their enthusiasm and confidence in life, thus providing significant assistance on a spiritual level.
“Usually I teach him, I say you need to have a good mindset, don’t think so much, because there are a few people in my village who are sick like this. But they don’t receive treatment in provincial hospitals, but in hospitals in their own counties, and now they have all lived for a few years, and it seems that they are also in the third stage, middle to late stage” (C3).
In Chinese culture, mutual assistance is considered a fine virtue, primarily manifested through helping each other during difficult times. This spirit of mutual aid is reflected in various social relationships, including within families, among friends, and across society at large. “That is, relatives and friends, they took the initiative to come and visit me, and there was that time when more than 20 classmates came, specifically to visit me, and each of them gave me 1,000 RMB (about US$141). They knew I had this disease and drove over specially” (P28).
Despite the importance of comfort from family and friends, they are sometimes not enough to fully alleviate a patient’s anxiety. Patients often harbor persistent concerns about the progression of their disease, and they crave more authoritative and specific reassurance and guidance from medical professionals.
“Now the doctor just says don’t think about it so much, and then he says how it’s so technologically advanced now. Anyway, the local doctor says don’t worry, you won’t die” (P19).
A patient was given a new lease of life because of the timely treatment by a medical professional, and this kindness was deeply rooted in his heart and that of his family members. This positive experience inspired his family to pass on this kindness and help to others, thus creating a positive chain reaction in society. It embodies the Confucian concepts of “benevolence” (ren) and “righteous conduct” (dao yì).
“The head nurse I’m really grateful to her, she saw [my situation] then rushed to call the doctor, said my situation is very bad and needs to be immediately rescued, no additional check-ups, open the green channel, directly into the operating room, that time is really to pick up a life back. Later, every time I came to the hospital, my wife would communicate with others, she would tell others about my life philosophy, the medicines I use, or the matching of the dietary aspects, and he would pass it on to others” (P28).
Missing companionship and challenges encountered by family and friends visiting the patient after surgery
As children start families, they are often separated from their families of origin. This spatial distance limits frequent contact and interaction between parents and children. As parents enter their later years, this separation can sometimes lead to them feeling isolated in terms of emotional and life support and facing the challenges of loneliness in old age.
“I have only one daughter she is married and we are the only two old people living in the house. The child has his own home and seldom comes to visit us” (C10).
“Because my grandchildren follow my son and daughter-in-law to study outside, I’m the only one in the house, and my partner died the year before” (P7).
During postoperative recovery, visits from family and friends are an important source of emotional support for patients. However, the challenge of geographic distance can be a barrier that prevents them from traveling to the hospital, thus limiting their opportunities to provide face-to-face care to patients.
“Family and friends are very concerned about us and call every day when they are free, so far away they can’t come even if they want to. Today my brother and sister-in-law both came to visit us in the morning, they are especially concerned about us, many friends wanted to come here to visit us, we thought it was too far to let them to come, it was inconvenient” (C27).
Caregiving burdens and challenges
Caregivers also experience significant psychological and physical stress in caring for their patients. This stress does not only stem from concerns about the patient’s health, but also from the fact that the caregiver has to perform multiple caregiving roles at the same time, especially in the middle-aged caregiver group. One interviewee described the dilemma of having to take time off work to care for his mother after a GC operation, while at the same time his two children were also in need of his care.
“As far as our family is concerned, my children are still in school, and we don’t have a high salary, and we are not bosses, we are just ordinary laborers. My mom’s health is not good either, she’s sick and suffering, and we’re worried. My two children are still young, she got sick, I suddenly rushed back, at least discharged from the hospital will be a period of time before I can go back, and now the two children in elementary school also have to pick up and drop off. It’s just a lot of trouble when I have to juggle all aspects” (C7).
Another middle-aged caregiver not only needed to work, but also needed to take care of his spouse and mother at the same time, as both had just undergone radical GC surgery. As a result, it was difficult for him to coordinate his schedule between work and caregiving tasks.
“I have to work every day and honestly it’s a little hard to coordinate. There are two people in my family [both with GC], this is my wife and (in the next bed) this is my mom” (C26).
Caregivers commonly report interruptions in their work as a result of taking on caregiving responsibilities. For example, a mother caregiver had to give up her job due to the need to provide long-term care for her young daughter with GC. In addition, caregiving had a significant impact on the quality of the caregiver’s sleep, which was often interrupted by medical procedures such as nighttime intravenous infusions. In more complex cases, balancing family responsibilities with caregiving tasks becomes even more difficult when the caregiver has health problems of their own. Together, these factors pose challenges to the physical and mental health of caregivers, affecting their daily functioning and QoL.
“I’ve never been in very good health, I’m always on medication, high cholesterol, I’m always on medication all year round anyway, basically non-stop…but then I have to find some work outside every day, to maintain the basic expenses of the family” (C21).
Caregivers face significant challenges in caring for their patients given their deficits in specialized caregiving skills. Therefore, in order to bridge this skills gap and ensure that patients receive the necessary quality of care, it is often necessary to hire additional specialized caregivers to assist. “We also hired a professional caregiver for three days because we didn’t understand so many things, and we were afraid of not taking good care of so many tubes on her” (C27). Additionally, considering the possible inconvenience of caregiving due to gender differences, one caregiver also hired a specialized caregiver to provide the necessary assistance. “A carer was hired to help, it’s sometimes inconvenient for me as a man and that’s when the carer helps” (C7).
Conceptual model
We created a loose conceptual model based on IFSMT and TDIM to categorize and visualize the facilitators or barriers identified. Since QoL was the main focus of this study, we used it as an outcome and linked the main results (Fig. 1). We identified new thematic categories based on existing theoretical frameworks, namely that comorbidities or unexpected events may alter the trajectory of pre-existing illnesses and increase the risk of disability or death as well as the psychological burden for patients. These factors may have an impact on the QoL of patients and their family caregivers. However, healthcare professionals tend to focus on the patient’s primary illness when treating them, ignoring the risks and harms that comorbidities may pose. In the past, the environment has been abstracted as the sum of the physical, psychological, natural and social environments. In this study we visualize environmental factors and specify the impact of medical environment, social assistance, economic and living environment on QoL of cancer families. Not only that, in this study we recognized the family unit as the sum of the patient and his/her family caregivers, and it was found that caregiver factors as part of family factors also have an impact on the patient’s QoL, and patient factors were similarly demonstrated to directly influence caregiver QoL. Knowledge and beliefs in the original theoretical framework stayed at the level of consciousness, and we provided an in-depth analysis of the knowledge and beliefs of GC patients and their family caregivers’ understanding of knowledge and beliefs and the mechanisms that shape them, viewing them more broadly as subjective behaviors driven by health awareness, medical decisions made under the guidance of HL, or lifestyles influenced by health perceptions. Unfortunately, we have not identified new self-regulatory factors. In exploring the area of social promotion, we specifically emphasized the importance of social support and the challenges it faces in practice. We recognize that caregiving burden is not only a family-level factor, but to a large extent reflects inadequate social support. Indeed, caregiving burden is often the result of a combination of social and external factors, not simply family characteristics. Ultimately, we include caregiving burden within the category of social facilitators. These factors interact and influence each other to some extent, and discussing the impact of one component on QoL in GC families in isolation is incomplete and inadequate. The present study goes beyond previous definitions of QoL in that the role of the caregiver is essential in cancer families.
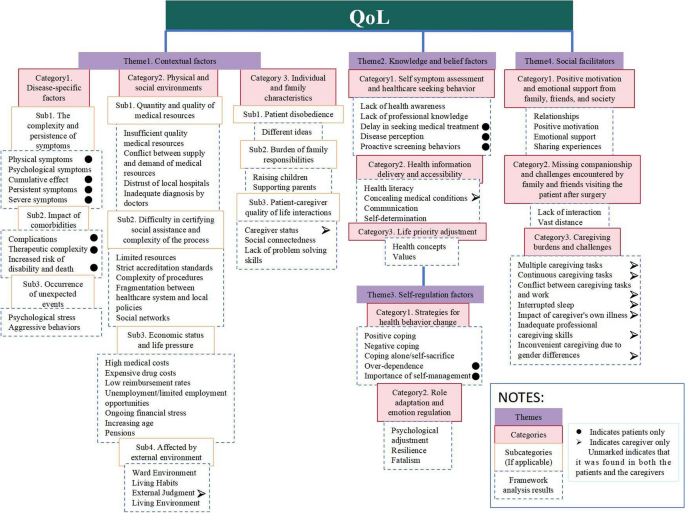
Model and framework analysis
link

